Olaf J. Rustad, MD
 Dr. O.J. Rustad completed his four year Dermatology residency program at the University of Minnesota. He then was selected for a Cutaneous Surgery Fellowship at the University of MN in 1990. During this fellowship, he received further extensive surgical training in Mohs skin cancer surgeries as well as cosmetic surgeries and procedures. This additional training has allowed him to develop proficiency in the various surgeries of the skin.
Dr. O.J. Rustad completed his four year Dermatology residency program at the University of Minnesota. He then was selected for a Cutaneous Surgery Fellowship at the University of MN in 1990. During this fellowship, he received further extensive surgical training in Mohs skin cancer surgeries as well as cosmetic surgeries and procedures. This additional training has allowed him to develop proficiency in the various surgeries of the skin.
After years of providing surgical treatments to patients from the outpatient surgical suites of local hospitals, Dr. O.J. Rustad has provided these outpatient surgeries from ADC’s on-site outpatient surgical suites since 2000. He has therefore been able to conveniently, regularly, and more cost effectively offer these services, including Mohs skin cancer surgery, directly at ADC.
Dr. O.J. Rustad has performed 8,000+ Mohs skin cancer surgeries, including their necessary reconstructions.
He and his staff enjoy providing this service for our patients as well as for the patients of other referring
health care providers, and believe this is a great asset to our community from our practice.
Dr. Rustad is a member of the American Society for Mohs Surgery (ASMS) and has been since 2000. This organization was established in 1990 to “promote the highest standards of patient care relating to Mohs surgery for the surgical removal of skin cancer and other appropriate malignancies: to establish quality assurance and regular peer review of Mohs surgeons…
The ASMS explains ”Mohs surgery is not only a tissue-sparing surgical treatment, it has the highest cure rate for skin cancers. Mohs surgery has been shown to be a highly effective treatment for certain types of skin cancer, with a cure rate of up to 99% for certain tumors. Due to the fact that the Mohs procedure is micrographically controlled, it provides the most precise method for removal of the cancerous tissue, while sparing the greatest amount of healthy tissue.
For this reason, Mohs surgery may result in a significantly smaller surgical defect and less noticeable scarring, as compared to other methods of skin cancer treatment. The Mohs procedure is recommended for skin cancer removal in anatomic areas where maximum preservation of healthy tissue is desirable for cosmetic and functional purposes. It may also be indicated for lesions that have recurred following prior treatment, or for lesions which have the greatest likelihood of recurrence.”
Learn More About Mohs Surgery and Skin Cancer Reconstruction Below!
Mohs Surgery
8,000 Mohs Skin Cancer Surgeries and counting…
Dr. OJ Rustad completed his four year Dermatology residency program at the University of Minnesota. He then was selected for a Cutaneous Surgery Fellowship at the University of MN in 1990. During this fellowship, he received further extensive surgical training in Mohs skin cancer surgeries as well as cosmetic surgeries and procedures. This additional training has allowed him to develop proficiency in the various surgeries of the skin.
Surgical Testimonial
“Not very often do you find a doctor of Dr. O. J. Rustad’s caliber. He is not only a highly skilled MOHS surgeon; he is also a very compassionate and caring individual. You are definitely in the best hands when he is your doctor.”
Janet E.
Shoreview, MN
Mohs Surgery
Mohs surgery is a specialized technique for removing skin cancers. Instead of taking a large amount of skin all around a skin cancer, and having a pathologist later examine it in order to try and make sure all the cancerous cells are gone, Mohs surgery removes the smallest amount of normal tissue possible. This is especially important in areas such as the face, where it’s important to have a good cosmetic outcome as well as remove the cancer.
In Mohs surgery, as the cancer is excised, each section is microscopically examined to determine if any cancer cells are still present. If any cells remain, only the cancer cells and as few as possible normal cells next to that area are removed.
American Society for Mohs Surgery – Patient FAQs
Is Mohs surgery the best treatment option for all skin cancers?
If you have any type of suspicious skin lesion you should seek evaluation by a dermatologist. If skin cancer is suspected, he or she may recommend and perform a biopsy. Mohs surgery may be recommended based on the type…Mohs Surgery Patient FAQ’s.
GentleCure
Skin Cancer Reconstruction
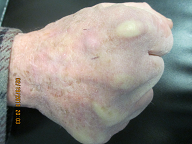
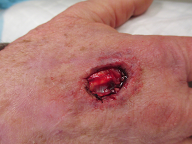
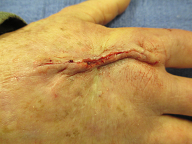
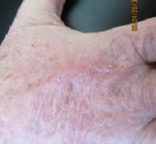
Skin Cancer on Right Hand – Squamous Cell Carcinoma (SCC)
Before Surgery Final Defect Closure One Month Post Op
Surgical Removal of Benign Lesions
In addition to cancer removal surgeries, Advanced Dermatology Care offers surgical excisions of benign lesions such as epidermal cysts, lipmoas, and warts. Like any surgery, an office visit to discuss options is required before scheduling any type of removal surgery.
Schedule an appointment today to learn about you options for a benign lesion removal!
Post-Surgical Care Instructions
Activity
Keep activity to a minimum for the first several days. Activity increases your blood pressure, which may lead to an increased tendency for bleeding, bruising and swelling, which may, in turn, increase pain and delay healing. Relax and recline for the first day or two following surgery. For surgery on leg(s) – will need to restrict from high-impact activity (running/jogging) for a few weeks after surgery to help keep stitches from breaking open. For surgery on upper body (back/arms)- Avoid high impact sports/golf/swimming for a few weeks-months depending on how large area is and the activity.
Eating
If surgery is performed around the lower part of the face (any area below the nose and above the neck), you should minimize talking and chewing. Eat soft or liquid foods for 2-3 days following surgery.
No Smoking
If you smoke, you should stop for both two weeks before, and after, surgery. Smoking causes blood vessels to constrict (get smaller), which decreases the blood supply, delays healing, and increases the likelihood of infection.
Pain
Post-operative pain is usually minimal. Plain or extra-strength acetaminophen (e.g. Tylenol), one to two tablets every four hours, usually relieves any pain you may have. You can also try over-the-counter topical Diclofenac 1% (e.g. Voltaren gel, Salonpas, Aspercreme, etc.). DO NOT TAKE ASPIRIN, IBUPROFEN, ADVIL, NUPRIN, ALEVE or NAPROXEN- if you have any questions, refer to the preoperative sheet or ask the doctor. Applying an ice pack over the dressing for twenty minutes every 2-3 hours during the first day will help minimize the swelling and bruising as well as lessen the pain. If your pain is not controlled by these measures, call us, and we will prescribe a pain medication for you.
Bleeding
Careful attention has been given to your wound to prevent bleeding. The dressing you have is a pressure dressing which will help prevent bleeding and minimize swelling. You may notice a small amount of blood on the edges of the dressing the first day. This is NORMAL.
If you develop bleeding that seems persistent, and soils the dressing, apply firm, steady pressure over the dressing with a gauze for FIFTEEN minutes without lifting the gauze. This is usually adequate treatment. If the bleeding persists, again apply firm pressure for another fifteen minutes. If it is still bleeding, call our office, try to call the doctor, or visit your nearest urgent care, emergency room or family physician.
Swelling & Bruising
This is common and temporary, usually lasting only 1-2 weeks. It is more common in areas treated around the eyes, hands, and feet, and is usually worse in the morning. To help minimize these complications, keep the affected areas elevated as much as possible. If surgery was done on your head, you should sleep with a couple of extra pillows under your head or mattress, elevate the head of your bed frame, or sleep in a recliner. Use of an ice pack and pressure dressing, as directed above, will help. After the third day, the use of warm, moist compresses may help speed the resolution of any residual swelling or bruising. For surgery on the legs- legs take longest to heal. You may notice increased swelling in or around the ankle as the fluid is retained there while on your feet- keep feet elevated above the level of your heart as much as possible. We will most likely be putting on a dressing called an Unna Boot on the leg that had surgery. You will need to come in once a week to have the Unna Boot changed, for up to 4 weeks. If an Unna Boot was applied, keep it DRY until your follow-up visit.
Infection
The suture line will be dark pink at first, and the edges of the wound will be reddened. This will lighten up day-by-day, and will become less tender. If the wound becomes increasingly red, swollen, inflamed, warm, painful, drains pus, or you develop a red streak, fever or chills, the wound may be infected. Please call our office immediately. The antibiotics you may be taking should help minimize the chance for an infection to occur. For surgery on the leg- legs take longer to heal and at times may require additional topical or oral medications.
Nerve changes
Numbness is usually temporary, but it may last for several weeks to months. You may also experience sharp pains or “zings” at the wound site as it heals as the nerve endings are re-connecting. This is normal and will gradually decrease in frequency. Occasionally, the nerve damage is permanent and sensation, or the capability to move certain muscles, is lost.
Itching
This is very common several days, to weeks, after surgery. This is a normal part of wound healing, but it is worsened by the stitches and dressing. Once these are removed, 4-14 days after surgery, there may be a significant reduction in symptoms. After stitches are removed, topical anti-itch medicine (ie: topical Benadryl) may be applied.
Wound Care
You may remove the dressing as instructed after surgery. You may shower and wash the area as usual. However, do not let the forceful stream of the shower hit the wound directly. After your shower, you can continue to practice the following wound care instructions until you have the sutures removed:
Initially, the wound may be tender and may bleed slightly, or seep a small amount of clear pale yellow to light greenish fluid. If these fluids dry, a crust, or scab, may form over the wound. Try not to allow this drying to occur as it leads to slower healing and increases the likelihood of scarring.
To prevent crusting, the suture line should be cleansed daily with warm, antibacterial soapy water (i.e. Dial, Cetaphil, Hibiclens) let the moisture loosen any crusts and remove drainage. You may help to gently loosen the crust with a cotton swab. Finally, pat the site dry. For stubborn crusting, place gauze soaked with water or hydrogen peroxide over the wound, allowing it to soak for five to ten minutes. Loosen and remove the debris gently. You may be instructed to clean your wound with Vinegar soaks instead of warm soapy antibacterial water. Mix over-the-counter distilled white vinegar with equal parts tap water. Soak for several minutes with soft cloth 1-2 times per day.
After cleaning, apply a thin layer of antibiotic ointment (e.g. Polysporin or Bacitracin, if not allergic to) to the wound. You may also use a silver spray (Element 47 can be obtained from ADC) and cover with Aquaphor or Vaseline. Cover the wound with a non-stick dressing (e.g. Telfa, Vigilon, etc.) and gauze. Tape the dressing in place. You may use a band-aid if the wound is small. Continue this process until your stitches are removed.
Call the office IMMEDIATELY if any of the following develop:
-
Excessive pain
-
Decreased vision, if your surgery was near your eyes
-
Any rise in temperature over 100* F
-
Excessive bleeding
-
Sudden swelling of forehead or eyes if surgery was on the face or scalp
-
Excessive redness and warmth around wound, and or drainage
Questions or Concerns
Please call our office at (651-484-2724) if you have any questions or concerns. If you need to reach someone after our usual office hours, you may attempt to reach Dr. Rustad by calling his cell phone (651-253-6926) from a touch-tone phone. If your call is not answered, please leave your name, number and a brief message at the tone. Your call will be returned as soon as possible. If your call does not get returned within several minutes, you should proceed to your nearest urgent care or emergency room.
Return to clinic as instructed for suture removal with medical support staff.
Return to clinic as instructed for follow-up office appointment with a provider.
If your insurance requires co-pay, one will be due at your follow-up office visit.






